GI-MAP Case Review for a Patient with Microscopic Colitis

When Conventional Treatment for Microscopic Colitis Fails to Resolve Symptoms
Sarah is a 45-year-old woman who presented to my clinic with chronic diarrhea and a host of diagnoses. She was diagnosed, by biopsy, with celiac disease at age 35 after suffering from chronic diarrhea for years. She began a very strict gluten-free diet which improved her energy but not her diarrhea. Sarah continued to have soft and unformed stools for the next six years. She returned to the gastroenterologist, and underwent an endoscopy and a colonoscopy, which revealed that she also had microscopic colitis.
Microscopic colitis is a chronic inflammatory disease of the colon that is characterized by chronic, watery, non-bloody diarrhea. It typically occurs in middle-aged patients and has a female preponderance. The colon appears typically normal or almost normal on colonoscopy in patients with microscopic colitis. The diagnosis is established by biopsy of the colonic mucosa demonstrating characteristic histologic changes.1 Standard of care for treatment of this condition is initiating a localized steroid like budesonide. My patient was prescribed budesonide and took it for six months.
Unfortunately, her symptoms didn't abate with the budesonide, and she continued to suffer from chronic diarrhea. Frustrated, she discontinued the medication. She scheduled an appointment to see me, and I immediately ordered a GI-MAP stool test to look for underlying causes of her symptoms unrelated to celiac disease or microscopic colitis.
The GI-MAP Revealed the Root Cause of Her GI Symptoms
When her GI-MAP test results came in, I immediately understood why Sarah was suffering with severe, chronic diarrhea for so long. She had three parasites detected, including Dientamoeba fragilis, Pentatrichomonas hominis, and Endolimax nana. Two of the three protozoa were lab high and orders of magnitude above reference range.
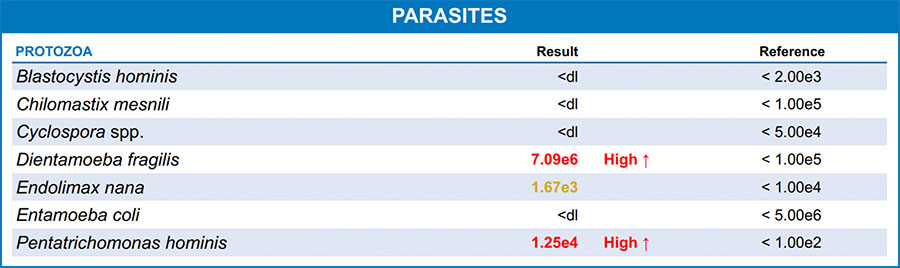
Further, nearly all of her fungal markers were elevated. Candida species were elevated, Candida albicans, Geotrichum spp., and Rhodotorula spp., were all elevated. Additionally, she had a suppressed Pancreatic Elastase 1 and a decreased secretory IgA.
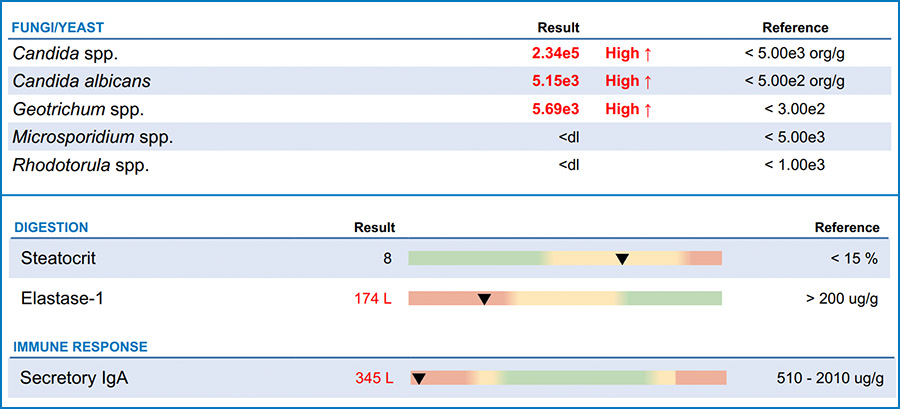
Looking at her symptoms and GI-MAP test results, I prioritized treatment of the protozoal species first. It has been my experience that the protozoa can change the makeup of the microbiome. Both Endolimax nana and Pentatrichomonas hominis fall under the category of commensal protozoa. In most people these parasites can be benign and not cause symptoms. Dientamoeba fragilis, however, can be symptomatic for many patients. It is an anaerobic intestinal protozoan parasite. Diarrhea, abdominal pain, flatulence, and anorexia are the most common symptoms seen with Dientamoeba fragilis.2
I prescribed a hybrid of both pharmaceutical and herbal interventions to treat Sarah. We prescribed two rounds of a five-day courses of nitazoxanide3 to target the Dientamoeba fragilis as well as an herbal product to target the yeast. The herbal products I prescribed were L-glutamine, allicin, cinnamon, N-acetyl glucosamine, and beta carotene.4
Microscopic Colitis That Doesn't Respond to Treatment Warrants a GI-MAP
Sarah responded very well to treatment. She went from having diarrhea many times throughout the day to having two formed bowel movements per day. Sarah remained on the anti-fungal treatment for three months. Subsequently, we were able to discontinue any digestive support without further incidence of chronic diarrhea.
Sarah's case is a very common case that we see in my office. Microscopic colitis is assumed to be present in 10–16 per 100,000 people. This condition has been on the rise for many years and has just recently plateaued.5 Patients often visit a functional medicine practitioner because they are unresponsive to standard care and are looking for other options. Using the GI-MAP's quantitative PCR (qPCR) technology, practitioners can get to the underlying cause of the chronic, unexplained symptoms. That was the case with Sarah — it's also the case for hundreds of other patients I treat.

Ilana Gurevich, ND, NSOM, FABNG
Dr. Gurevich is a naturopathic medical physician and an acupuncturist who uses individualized natural therapies to address the underlying cause of disease. She encourages her patients to take an active role in their own health care. Dr. Gurevich relies on a variety of natural modalities including Chinese and Western herbal medicine, acupuncture, nutritional supplements, homeopathy, hydrotherapy, and dietary education.
REFERENCES
- Christoph F Dietrich, MD, MBA. Microscopic (lymphocytic and collagenous) colitis: Clinical manifestations, diagnosis, and management. UpToDate. https://www.uptodate.com/contents/microscopic-lymphocytic-and-collagenous-colitis-clinical-manifestations-diagnosis-and-management
- Johnson EH, Windsor JJ, Clark CG. Emerging from obscurity: biological, clinical, and diagnostic aspects of Dientamoeba fragilis. Clin Microbiol Rev. 2004
- Nagata N, Marriott D, Harkness J, Ellis JT, Stark D. In vitro susceptibility testing of Dientamoeba fragilis. Antimicrob Agents Chemother. 2012;56(1):487. Epub 2011 Oct 24.
- Rohilla S, Bhatt DC, Gupta A. Therapeutic Potential of Phytomedicines and Novel Polymeric Strategies for Significant Management of Candidiasis. Curr Pharm Des. 2018;24(16):1748-1765. doi: 10.2174/1381612824666180524102933. PMID: 29792138.
- Tong J, Zheng Q, Zhang C, Lo R, Shen J, Ran Z Incidence, prevalence, and temporal trends of microscopic colitis: a systematic review and meta-analysis. Am J Gastroenterol. 2015;110(2):265. Epub 2015 Jan 27.