Zonulin and Autism: Tracking Intestinal Barrier Integrity with GI-MAP®

Autism Spectrum Disorder (ASD) is often described through behavioral criteria — but for many clinicians and families, the question remains: What underlying physiological changes may be contributing to these shifts?
Zonulin is a key regulator of intestinal permeability and is commonly used as a biomarker of gut barrier function. Elevated levels are associated with increased intestinal permeability, which may influence immune activity and systemic physiology. Interest in the relationship between gut permeability and autism has grown, particularly in patients presenting with gastrointestinal symptoms or restrictive eating patterns.
This case explores how GI‑MAP® stool testing was used to monitor intestinal barrier integrity over time, and how changes in zonulin aligned with changes in behavior and daily functioning.
What is Zonulin and How is it Related to Autism?
Zonulin is a key regulator of intestinal permeability. Elevated zonulin levels are associated with increased intestinal permeability, often referred to as “leaky gut.” In autism, increased intestinal permeability has been explored as a potential contributor to gastrointestinal and systemic symptoms, although research is ongoing.
Patient Overview
Until approximately 19 months of age, this patient’s development appeared typical. She was a joyful and expressive child who played with her older sister and responded naturally to the world around her.
Then, subtle but concerning changes began to appear.
She gradually stopped communicating as she had before. Her eye contact diminished, and she became increasingly withdrawn from her surroundings. She no longer wanted to play with her sister and often seemed disconnected from the environment around her.
Her eating patterns also changed. She became extremely selective, favoring simple carbohydrates and sweets. At the same time, new behaviors emerged, including mouthing non-food items such as paper and tissue.
Over time, the few words she had developed disappeared. Eventually, she stopped speaking altogether.
A comprehensive developmental evaluation later confirmed a diagnosis of autism spectrum disorder. These changes raised an important clinical question: Could underlying biological processes be contributing to what was being observed behaviorally?
This question led me to begin investigating metabolic, nutritional, and gastrointestinal factors using advanced laboratory testing.
The Role of GI‑MAP in Evaluating Gut Health and Intestinal Permeability
To explore possible physiological contributors, a comprehensive laboratory evaluation was performed, including a GI‑MAP stool analysis.
GI-MAP stool testing offers a functional assessment of the gastrointestinal environment, including:
- Microbiome composition
- Immune activity within the gut
- Inflammatory markers
- Markers of intestinal barrier integrity, including zonulin
In this case, GI-MAP was not used as a single snapshot, but as a longitudinal tool — allowing patterns to emerge over time.
Zonulin and Intestinal Permeability in Autism
Zonulin levels were tracked across multiple GI-MAP tests.
Over time, a consistent pattern became apparent:
- When zonulin levels increased, behavioral restlessness was more pronounced
- As zonulin levels decreased toward the reference range, improvements in calmness and daily functioning were observed
Representative Results:
- Test One - Zonulin: 315.9 ng/g (Reference <175)
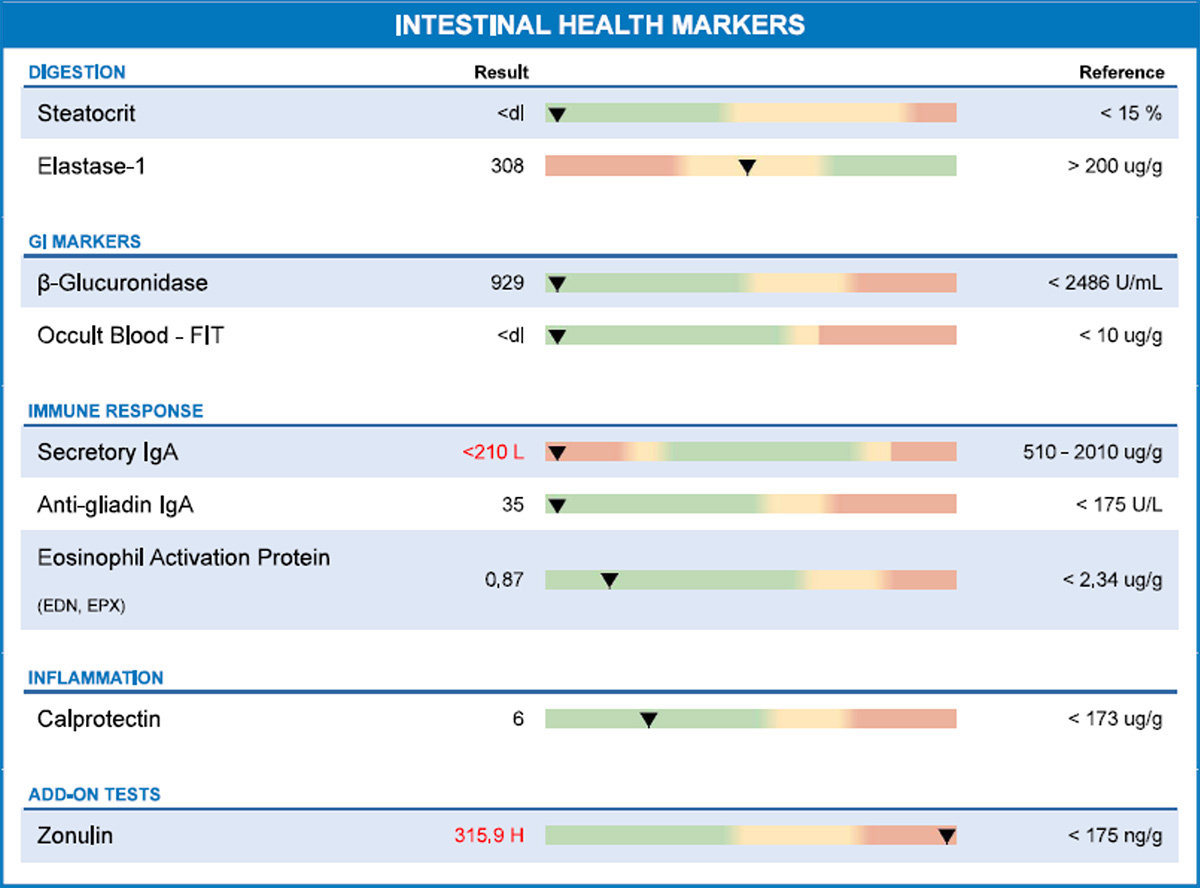
- Test Two - Zonulin: 244.2 ng/g
In a subsequent test performed several months later, zonulin levels had decreased but were still above the reference range.
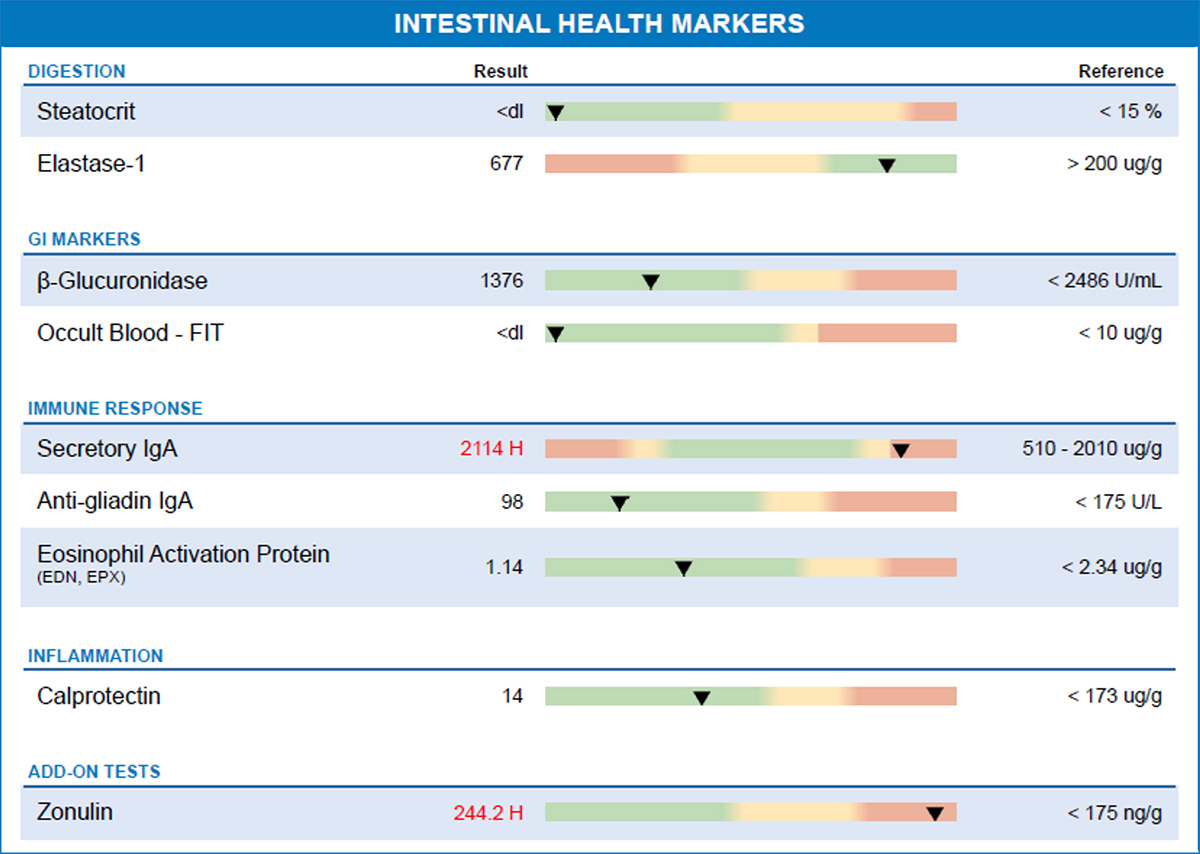
- Test 3 - Zonulin: 106.4 ng/g (within reference range)
In a later follow-up test, zonulin levels had decreased further.
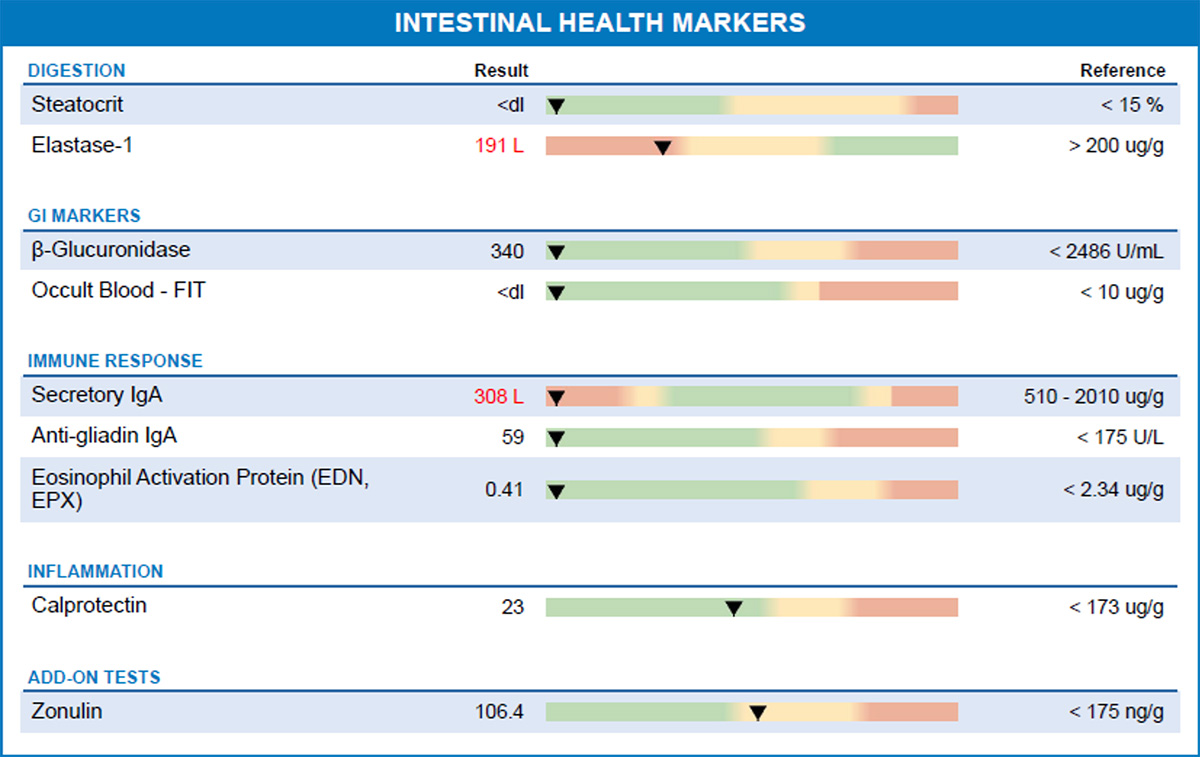
Within a period of several months, zonulin levels had normalized.
Tracking zonulin over time provided insight into changes in intestinal barrier function that would not be captured by a single time measurement. These observations highlight the importance of longitudinal monitoring of intestinal barrier markers, as changes may occur alongside behavioral shifts.
Clinical Approach
Based on the findings, intervention focused on supporting intestinal barrier integrity and maintaining microbiome balance through personalized nutritional and metabolic support.
GI-MAP findings, including zonulin trends, were used to guide and adjust the clinical approach over time.
Observed Clinical Changes
Alongside GI-MAP improvements, the patient experienced meaningful changes in daily functioning.
These included:
- Improved eye contact
- Increased social engagement
- Gradual return of communication abilities
- Greater emotional expression
Clinical Summary
- Zonulin is a marker of intestinal permeability measurable on GI-MAP stool testing
- In this case, elevated zonulin levels were observed alongside increased behavioral dysregulation
- Decreasing zonulin levels over time aligned with improvements in daily functioning
- Longitudinal GI-MAP testing provided clinical context not visible from a single measurement
Key Takeaways
The intestinal barrier plays a central role in immune signaling and systemic physiology.
In this case, tracking zonulin levels over time provided a useful biological marker for observing changes in intestinal barrier integrity, highlighting the potential value of integrating GI-MAP stool testing into the ongoing assessment of complex conditions such as ASD.
By using GI-MAP to track markers like zonulin over time, clinicians may gain:
- Greater visibility into intestinal barrier function
- A framework for observing physiological trends
- Additional context for clinical decision-making
Additional Resources
For clinicians interested in further exploring intestinal permeability and zonulin in clinical practice:
- GI-MAP Interpretive Guide – Additional markers and patterns related to intestinal permeability can be found in Table 21a (Gut Barrier Permeability “Leaky Gut” Pattern).
- DSL Academy Zonulin Module — A detailed overview of zonulin as a marker of intestinal permeability and its role in gut barrier function.
- Webinar: Beyond Leaky Gut — A clinical overview of intestinal permeability and interpretation of gut barrier markers.

Tali Engor, B.Sc.Pharm, B.Sc. Pharmaceutical Chemistry
Tali Engor, B.Sc.Pharm, B.Sc. Pharmaceutical Chemistry, is a pharmacist and pharmaceutical chemist whose professional work was shaped by her personal journey as the mother of a child diagnosed with Autism Spectrum Disorder (ASD).
Her academic training includes a Bachelor of Science in Pharmacy (B.Sc.Pharm) from the Faculty of Medicine at the Hebrew University of Jerusalem and a Bachelor of Science (B.Sc.) in Pharmaceutical Chemistry from Bar-Ilan University.
Beyond her core academic degrees, Engor completed additional professional training in integrative autism approaches, naturopathic studies, and clinical disciplines including psychiatry and neurology. She previously served as a council member of the Pharmaceutical Society of Israel. To learn more about the development of the C.A.T. Method, see The Story Behind C.A.T.
natautism.com/en/the-story-behind-cat
The opinions expressed in this presentation are the author's own. Information is provided for informational purposes only and is not meant to be a substitute for personal advice provided by a doctor or other qualified health care professional. Patients should not use the information contained herein for diagnosing a health or fitness problem or disease. Patients should always consult with a doctor or other health care professional for medical advice or information about diagnosis and treatment.